KPIs to Fit Your 2020 Challenges as a CFO


Hospital CFOs are facing challenges that are becoming more complex and increasingly tied to other organizational initiatives. As your organization addresses new forms of competition, navigates the consumerization of healthcare, and finds its way in the wake of new payment and medical billing practices, it will be crucial to pinpoint the KPIs that align with your goals.
To stay ahead of the curve and focus on the future, we’ve put together this challenge-based list of KPIs (MAP Keys included) to prioritize in 2020.
1. Cash Flows & Collections
A staple indicator of revenue cycle health, these KPIs will keep you on top of red flags in cash flows and collections activities.
1.1. Bad Debt (AR-7)
This KPI is useful for judging the effectiveness of financial counseling and collection efforts.
Equation:

1.2 Aged A/R as a Percentage of Billed A/R by Payer Group (AR-2)
This KPI provides valuable insight and indicates revenue cycle effectiveness in terms of liquidating A/R by payer group.
Equation:

2. Revenue Cycle Performance
2.1. Net Days in Accounts Receivable (FM-1)
This is a good trending indicator of overall A/R performance that points back to revenue cycle efficiency.
Equation:

2.2. Aged A/R as a Percentage of Total Billed A/R (AR-1)
This trending indicator reflects receivable aging and collectability and points to revenue cycle effectiveness at liquidating A/R.
Equation:
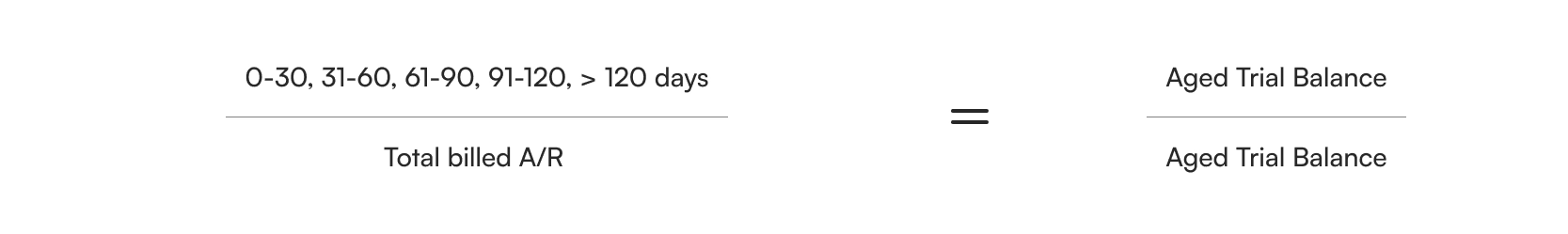
2.3. Aged A/R as a Percentage of Total A/R (AR-3)
Another trending indicator of receivable aging and collectability.
Equation:

3. Denial Management
Denial management will become increasingly important as coding remains complex and payers tighten their guidelines.
3.1. Denial Write-offs as a Percentage of Net Patient Service Revenue (AR-6)
This is a staple of denial KPIs and worth monitoring after software upgrades, and changes to medical billing processes, or contractual relationships.
Equation:

3.2. Remittance Denial Rate (AR-5)
This KPI is also an efficiency and quality indicator.
Equation:

4. Identifying Opportunities
Modern CFOs move beyond monitoring and scan for opportunities in front of them.
4.1. Late Charges as a Percentage of Total Charges (CL-2)
This KPI reveals opportunities to reduce unnecessary costs, accelerate cash flows, and improve revenue capture.
Equation:

5. Data Governance & Data Quality
CFOs have growing data challenges so clean claims and data quality KPIs will only become more important with time. As you implement new revenue cycle technologies, these KPIs will be especially useful in maintaining data governance standards.
5.1. Clean Claim Rate (CL-1)
Equation:

6. Clinical Reporting
If you’ve brought on any new software or procedures for your clinicians, this KPI will be especially useful.
6.1. Case Mix Index (FM-5)
Equation:

7. Self-Pay Insights
Patients are now the biggest payer groups behind Medicare and Medicaid, meaning that self-pay KPIs should likely move up on your list of priorities. These KPIs highlight the self-pay gross revenue that isn’t included in your cash, charity, or bad debt metrics.
7.1. Uncompensated Care (FM-4)
Equation:

7.2. Uninsured Discount (FM-3)
Equation:

8. Overall Financial Health
This KPI is a trending indicator of your ability to turn net patient services into cash and points to the fiscal integrity of your organization.
Equation:

If you’d like guidance in prioritizing your hospital KPIs for this year and would like to learn more about the services we offer, start here.
[1] M. Korolov, "Black market medical record prices drop to under $10, criminals switch to ransomware," CSO, 23 December 2016. Available: https://www.csoonline.com/article/3152787/black-market-medical-record-prices-drop-to-under-10-criminals-switch-to-ransomware.html.
[2] L. Columbus, "58% Of All Healthcare Breaches Are Initiated By Insiders," Forbes, 31 August 2018. Available: https://www.forbes.com/sites/louiscolumbus/2018/08/31/58-of-all-healthcare-breaches-are-initiated-by-insiders/?sh=7eee42ed601a.
[3] U.S. Department of Health & Human Services, "Covered Entities and Business Associates". Available: https://www.hhs.gov/hipaa/for-professionals/covered-entities/index.html.
[4] U.S. Centers for Medicare & Medicaid Services, "Are You a Covered Entity?". Available: https://www.cms.gov/Regulations-and-Guidance/Administrative-Simplification/HIPAA-ACA/AreYouaCoveredEntity.
Are Your 2020 KPIs Aligned to Tackle Hospital CFO Challenges?
Get expert guidance on prioritizing KPIs to strengthen your hospital’s revenue cycle and financial performance.


Connect with our experts to:
- Identify KPIs that optimize cash flow, denials, and revenue cycle performance.
- Improve data quality, clean claim rates, and reporting accuracy.
- Gain actionable insights to reduce administrative costs and enhance financial health.
Explore our strategic insights & resources
FAQs
The FAQ section simplifies key information about 3Gen Consulting’s services, helping partners navigate our offerings, methodologies, and value.
KPIs provide actionable insight into cash flow, denials, and operational efficiency, helping CFOs make informed financial decisions.
Monitoring Aged A/R and net days in A/R identifies collection inefficiencies, accelerates cash flow, and reduces bad debt.





